
That portion of the visit must be medically necessary and reasonable to treat the patient’s illness or injury or to improve the functioning of a malformed body part.ĬPT only copyright 2022 American Medical Association. When you provide an IPPE and a significant, separately identifiable, medically necessary Evaluation and Management (E/M) service, we may pay for the additional service. Qualified non-physician practitioner (NPP) (physician assistant, nurse practitioner, or certified clinical nurse specialist ).Physician (doctor of medicine or osteopathy).Part B covers an IPPE when performed by a: We don’t require you to use a specific IPPE diagnosis code, so you may choose any diagnosis code consistent with the patient’s exam. 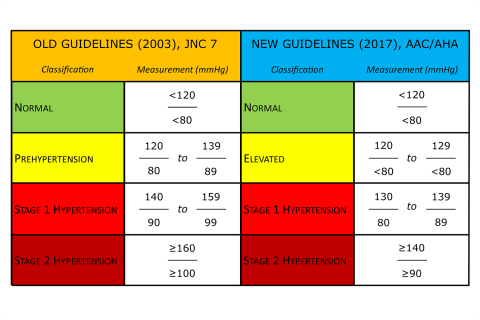 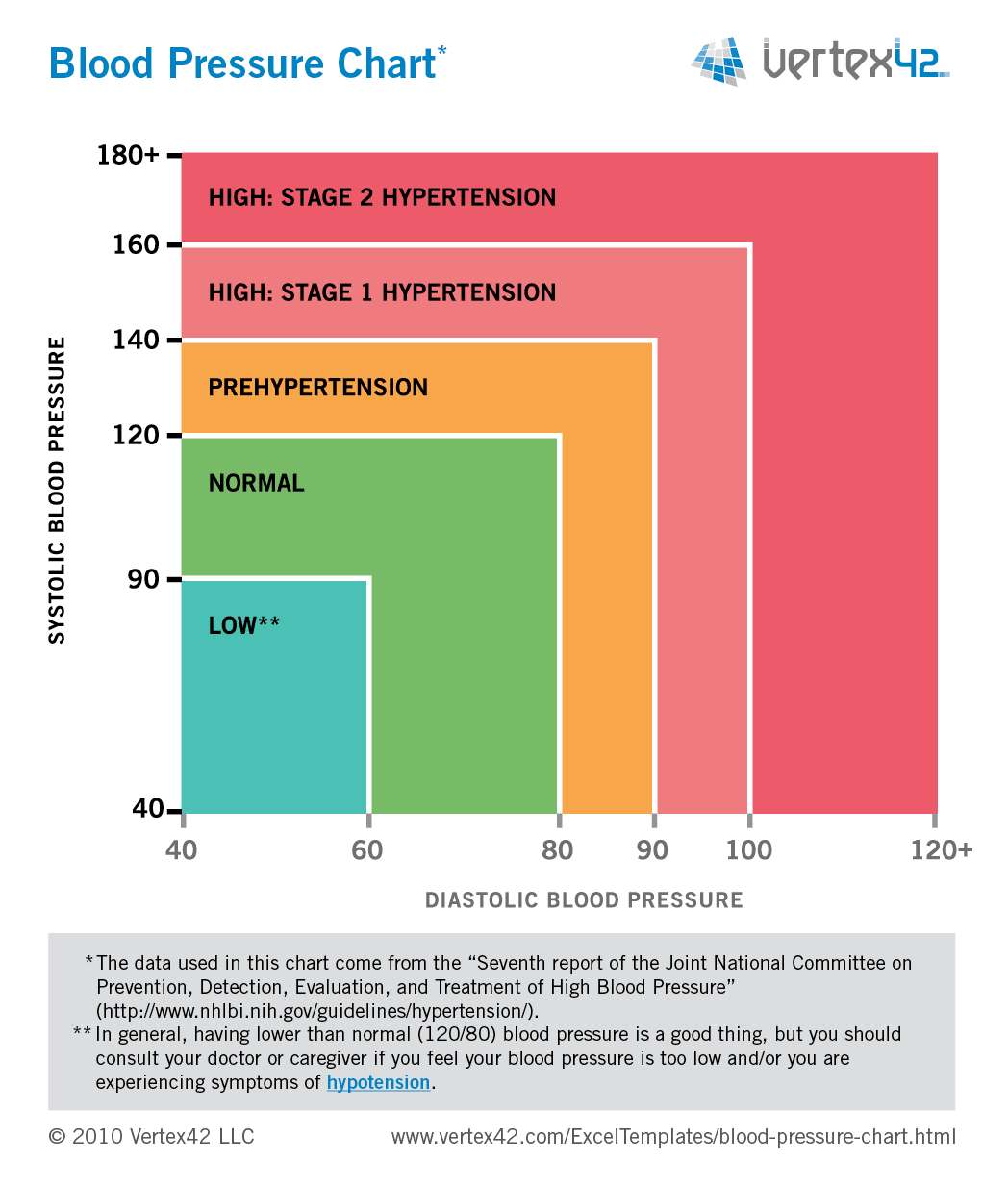
You must report a diagnosis code when submitting IPPE claims. 
* Section 60.2 of Medicare Claims Processing Manual, Chapter 9 has more information on how to bill HCPCS code G0468. Federally qualified health center (fqhc) visit, ippe or awv a fqhc visit that includes an initial preventive physical examination (ippe) or annual wellness visit (awv) and includes a typical bundle of medicare-covered services that would be furnished per diem to a patient receiving an ippe or awv
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
